When you’re eligible to delay enrollment in Medicare because you have creditable employer coverage (through your employer or a spouse’s employer) you qualify for an 8-month Special Enrollment Period (SEP). During this time, you’ll be able to enroll in Medicare.
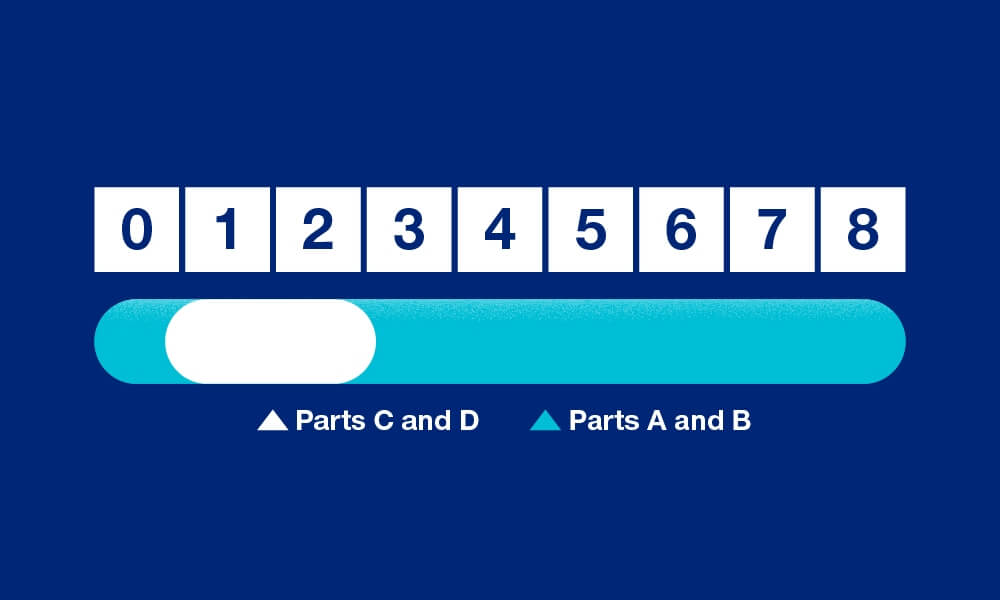
Your Special Enrollment Period begins when you retire or lose your employer coverage, whichever happens first. You will have up to 8 months to enroll in Parts A and/or B, but only the first two months to enroll in Parts C and/or D.
How to use your Special Enrollment Period
When you’re ready to enroll in Medicare, you will have a full 8 months to enroll in Parts A and/or B but only the first two months of this period to enroll in Parts C and/or D. Watch the video below to help you understand how to enroll during your Special Enrollment Period after you lose employer coverage or stop working.
When to enroll in Medicare if you worked past 65

Upbeat music plays. An illustration of a light blue briefcase appears against a deep blue background. Text appears as a Narrator speaks in voiceover.
ONSCREEN TEXT: Medicare Special Enrollment Period: Working Past 65
NARRATOR: Medicare special enrollment for people working past sixty-five.
A speech bubble rises from an illustration of a person with blonde hair.
ONSCREEN TEXT: Who can qualify?
NARRATOR: Who can qualify.
The briefcase and person slide out of sight. The head of a dark-haired person, and a sheet of paper that reads, “Creditable employer coverage,” slide into view.
ONSCREEN TEXT: Individuals with creditable employer coverage
NARRATOR: Individuals working past sixty-five with creditable employer health coverage…
The sheet of paper disappears. The head of a blonde person slides beside the dark-haired person’s head, along with an illustration of two side-by-side buildings.
ONSCREEN TEXT: Individuals covered by spouse’s creditable employer coverage
NARRATOR: …and individuals covered by a spouse’s creditable employer plan, who are not required by the employer to take Medicare at age sixty-five in order to remain a covered dependent.
The people slide out of view, and the number “20+” appears beside the illustrated buildings.
ONSCREEN TEXT: Employer must have 20 or more employees in both cases
NARRATOR: In both cases, the employer providing the health coverage must have twenty or more, employees.
Eight calendars appear in two rows.
ONSCREEN TEXT: Special Enrollment Period 8 months Dates vary by person
NARRATOR: Your special enrollment period begins the month after you leave your job, or lose your employer coverage, and lasts for eight months.
Illustrated icons of a bed and stethoscope respectively labeled “Part A” and “Part B” appear.
ONSCREEN TEXT: 8 months to get Part A & Part B
NARRATOR: You’ll have the full eight months to enroll in Medicare Part A and Part B.
An icon of a bed and stethoscope labeled “Part C” appears beside an icon of a prescription bottle labeled “Part D.”
NARRATOR: But be careful. You only have the first two months to enroll in Medicare Part C, or Part D, without penalty.
Blue text appears against a white background.
ONSCREEN TEXT: Medicare Made Clear brought to you by UnitedHealthcare
©2022 United HealthCare Services, Inc. All rights reserved. Medicare Made Clear® by UnitedHealthcare® Y0066_SEPWP65_C
A swirl of blue ribbons turn into the stacked blue U’s of the UnitedHealthcare logo, then fade to text.
ONSCREEN TEXT: United Healthcare
During your Special Enrollment Period, you have 8 months to enroll in Part B, and Part A, if you haven’t already, and you will have 2 months to enroll in a Medicare Advantage (Part C) or a Part D prescription drug plan.

An important note about Part D: You have exactly 63 days to get a stand-alone Part D prescription drug plan or a Medicare Advantage plan with prescription drug coverage included without penalty. After this time, you may be subject to the Part D late enrollment penalty which generally lasts as long as you have Medicare prescription drug coverage.
Finally, it is important to know that you are not eligible for this Special Enrollment Period when your COBRA or retiree coverage ends. However, you may be eligible for a different Special Enrollment Period specific to a qualifying life event.
About Medicare Made Clear
Medicare Made Clear brought to you by UnitedHealthcare provides Medicare education so you can make informed decisions about your health and Medicare coverage.
Get the latest
Boost your Medicare know-how with the reliable, up-to-date news and information delivered to your inbox every month.
*All fields required